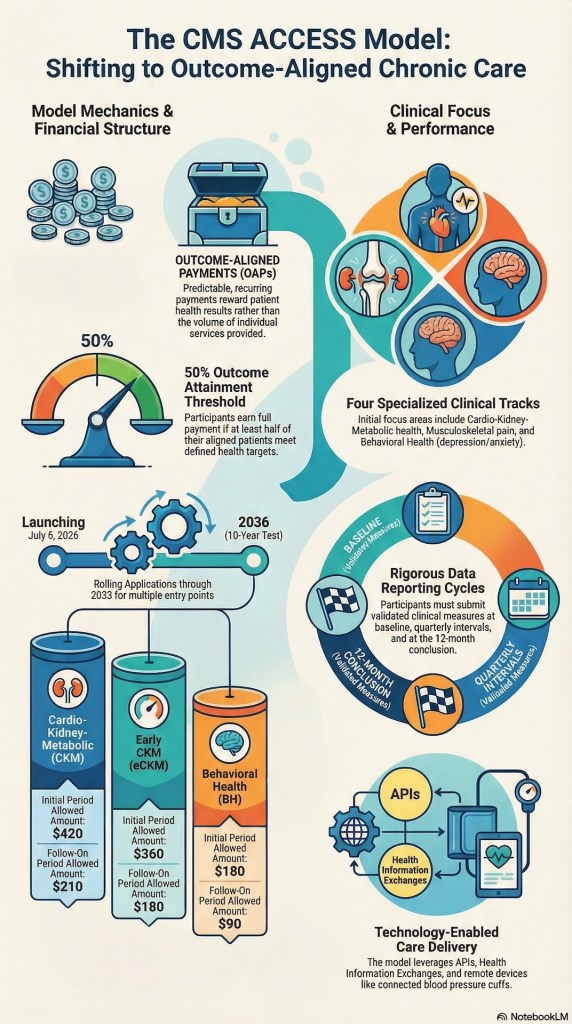
A new value-based care model arrives from Washington. Set to replace ACO REACH in 2027, the Long-term Enhanced ACO Design (LEAD) is touted as the ultimate solution to unsustainable national healthcare costs and primary care physician burnout. But is it truly a tool for independent practice survival, or merely a sophisticated engine for corporate consolidation?
⚖️ The Math of Independence
CMS built LEAD to counter the privatization of Medicare via Medicare Advantage (MA) and stabilize small ACOs. But understanding the implications requires looking past the promises and examining the actuarial math.
The Mechanics of LEAD
To understand the strategic shift, we must examine the four foundational rules of the LEAD model that transform traditional ACOs into “Payviders”—entities holding global financial risk while Medicare transitions into a Third-Party Administrator (TPA) role.
10-Year Horizon
Running from 2027 to 2036. Crucially, there is no rebasing, meaning ACOs won’t be punished with lower benchmarks for being efficient early on.
Global Risk
ACOs take on 100% upside and downside financial risk, accompanied by prospective, capitated population-based payments.
CARA Integration
A disruptive mechanism allowing ACOs to create episode-based risk agreements with specialists, with CMS acting as the middleman.
Patient Persuasion
Global ACOs get tools to buy loyalty (Part B cost-sharing support, Part D premiums), essential since patients retain full freedom of choice.
The Paradigm Shift: Medicare as a TPA
By handing over 100% global risk and upfront capitation, CMS is fundamentally changing its relationship with the delivery system. Health organizations are no longer just treating patients; they are absorbing the insurance risk, while Medicare steps back into an administrative role.
CMS / Medicare
- Processes FFS Claims
- Sets Financial Benchmarks
- Monitors Compliance
& Upfront Capitation
Health Organization
- Holds Global Financial Risk
- Manages Specialists (CARA)
- Designs Care & Benefits
Transitioning health systems into risk-bearing “Payviders” places them directly into the arena with commercial insurance titans. This sets up the inevitable clash: ACO LEAD vs. Medicare Advantage.
The Battleground: MA vs. LEAD
While clinical goals align between health plans and ACOs, their operational engines are entirely different. This visualization contrasts their approaches to controlling care and capturing revenue.
Medicare Advantage (MA)
Commercial insurers extract profit margins before delegating risk. They rely on administrative friction.
ACO LEAD (Global)
CMS bypasses the commercial insurer entirely. ACOs must use clinical coordination, not friction.
Corporate Gamification
CMS actuaries built the 10-year LEAD math to kill “junior-varsity” games like simple upcoding. However, large corporate health systems play an advanced, multi-layered game of structural arbitrage that small practices cannot access.
System Arbitrage
To a hospital CFO, the ACO can run at a deficit for years, so long as it acts as a clinical vacuum, pulling patients into the high-margin hospital FFS ecosystem.
Ancillary Arbitrage
The real margin is in lab, imaging, and specialty pharmacy. Systems use EMR workflows to retain 95%+ of that high-margin business internally.
Regulatory Arbitrage
Small practices follow the rules. Large systems deploy armies of lobbyists to D.C. to adjust benchmark formulas in their favor before a single claim is filed.
The Inevitable Squeeze
Despite genuine attempts to lower the drawbridge, frontline doctors will still get squeezed. This chart illustrates how the hard-earned “Shared Savings” are distributed.
Where does $100 of Shared Savings Go?
Inside a hospital ACO, employed PCPs face a dual mandate. If you keep a patient healthy, the hospital pockets the shared savings, but you lose FFS income. You do the work; the corporation captures the upside.
Physician-led ACOs generate higher savings, but lack capital for LEAD’s risk reserves. To survive, they hire a tech enabler, trading half of their savings to a venture-backed middleman just to play the game.
“By transforming hospital systems into massive, risk-bearing ‘Payviders,’ LEAD leaves private practice with an impossible ultimatum: